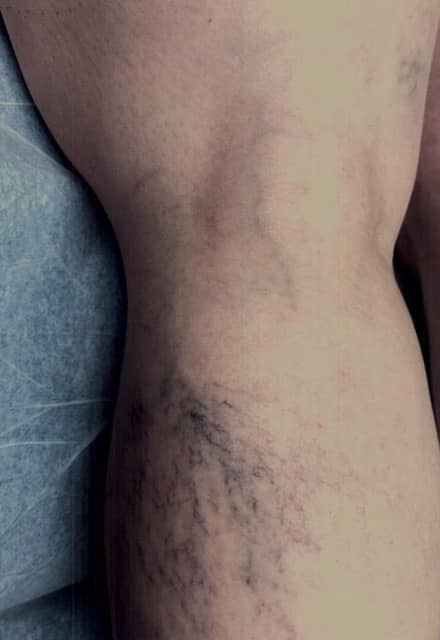
Most of the time diagnosis of spider veins is straightforward. There they are on your legs. But it is important to identify associated vein disease. Are there also varicose veins present? We have many patients asking to have spider veins treated, yet ignore their varicose veins. In general, this will not produce a satisfactory outcome. The underlying factors causing the varicose veins usually relate to the spider veins as well. Usually, one must treat the varicose veins first before treating the spider veins. If spider veins are very extensive, or form dark purple clusters, an underlying vein abnormality must be sought, and, if identified, treated prior to spider vein treatment. So, sometimes a patient interested in having spider vein treatment may need to have an ultrasound examination to evaluate these special situations.
It is also important to identify other factors which may influence spider vein Vein Disorders – Varicose Veins treatment. Has there been prior vein treatment, and, if so, any complication from it? Was there a significant injury or major surgery of that leg that could have disrupted normal vein patterns? Does the patient have other chronic conditions, blood disorders, autoimmune diseases, diabetes, arterial disease, obesity, skin conditions, etc.? Is the patient taking any medications that could influence treatment, such as blood thinners, steroids, antibiotics, etc.? So, even though treatment of spider veins seems simple, it is important that is supervised by a physician specialist in vein disease.
Sclerotherapy involves the injection of solutions into the veins that cause them to shut down by a process similar to scarring. The needle used is very tiny, and even people with a history of fear of needles tolerate the procedure well. The solutions do not harm other organs in the body, and have longstanding safety records. Highly concentrated saline has been used by many physicians, but is very painful. Most experts use solutions that are chemically similar to detergents. These cause only minor discomfort, and generally give better results. Severe allergic reactions to these solutions have been reported, but are very rare. At an international meeting of vein experts, physicians were asked if they had ever seen a serious allergic reaction with use of any of these solutions. Not one hand was raised. If there is a risk from allergic reaction, it must be very, very small. In over 20 years experience with sclerotherapy, I have seen only a few patients with allergic reaction.
Prior to treating the spider veins directly, any associated vein abnormalities must be addressed. At a minimum, this usually involves injection of feeder veins, called reticular veins, and we consider this the first step in treating spider veins. Omitting this is the most common reason we see for poor results in patients treated elsewhere for their spider veins. After a minimum of three weeks following treating the reticular veins, the spider veins themselves can be treated. We usually check the results of this after another three weeks, and do touch up injection of any spider veins that do not appear to have been treated. So, the first spider vein treatment usually takes two or three steps. After each injection session a compression stocking is worn overnight.
What is said here applies to use of laser in treating spider veins of the legs. Lasers are often used to treat spider veins of the face and trunk, and seem very appropriate for that. Treating leg veins is a different matter. Lasers may treat surface spiders as effectively as sclerotherapy. That’s the best that can be said. There is no evidence to suggest lasers are more effective than sclerotherapy. The advantage for physicians who use laser on spider veins is that it is very easy to do. Often, however, in the hands of a non-specialist, reticular veins and other vein disorders are not treated, and the results can be sub-optimal. Lasers are often promoted as being able to treat veins that are too small to be injected. There is no such thing as too small a vein for someone experienced in sclerotherapy. People who have had both laser treatment and sclerotherapy report that laser is more painful. That surprises many people, but when you think laser, remember you are thinking about destruction of veins. Remember what lasers did in the last James Bond movie you saw. Laser treatment is more expensive than sclerotherapy because the technology is more expensive. To sum it up, laser hurts more, costs more, and is no more effective, and often less effective than sclerotherapy. Which one to choose seems obvious. Most specialists in vein disease use sclerotherapy rather than laser in treatment of spider veins of the legs.
After completing the treatment process enough time should be allowed to give the healing process an opportunity to yield the best result. Treatment for vein disease is a process rather than an event. Sometimes there is improvement in the appearance of spider veins after just treating the reticular veins. Sometimes the treated spider veins rapidly become fainter within a week or two. Sometimes substantial improvement takes 6-8 weeks. There will be continued improvement, however, over several months. We usually predict that pink spider veins may become unnoticeable, red ones may become pink, and purple ones may become red or just less prominent purple. It is important to understand that the treatment is not a miracle. We usually suggest waiting three to six months before re-treating remaining spider veins in order to get the most out of the first treatment efforts. Treatment for remaining spider veins usually entails a single injection, since the feeding veins have already been treated. When treating especially dark purple spider veins, two or three treatments over nine to twelve months may be necessary. Also, people with extensive spider veins may not be able to have them all treated in a single session; there are safety considerations in how much solution may be injected at one time. So, remember, you took a lifetime to develop these veins; give us some time to get rid of them. The longer treatment has been delayed, and the more extensive and dark the spider veins, the more involved treatment will be, and the longer it will take to get a good result. Just as one straightens one’s teeth through a process of wearing braces, so getting rid of spider veins means getting into the process. Fortunately, it’s not as long as wearing braces. And the sooner you start the process, the sooner you’ll be wearing shorts again.
Most of the possible problems that can occur with sclerotherapy are more nuisance than a threat to life or health. Sclerotherapy is medical procedure, and should be carried out under the responsibility of a physician with training and experience in venous disease. While problems in treatment of spider veins are usually not serious, it is important to be aware of several possible events.
- The most important possibility is development of blood clots in the deep veins of the leg that can travel to the heart. This is very a rare occurrence, and has not happened in any of the patients I have treated. We stick to safety recommendations to limit how much solution we will inject at a session in order to avoid any risk of deep vein clots. It is very important to let us know if you or any family member has had a history of blood clots in the leg veins.
- Very rarely sclerotherapy may result in the breakdown of a small area of skin resulting in a small open wound. These eventually heal, usually with minimal cosmetic problem. People who have any condition which contributes to slow wound healing are at risk for this complication.
- Staining is the most common side-effect of sclerotherapy. This refers to the development of tan or brown discoloration in the skin over the injected veins. Most of the time, this occurs as a result of the healing process. Sometimes blood trapped in the effected vein can cause deposition of blood pigments in the skin and produce staining. Staining usually disappears (though it may take over a year in some people). People with darker skin pigmentation may be at higher risk for staining, so we usually start treatment in those cases by injecting a small test area.
- Blushing or matting refers to the development of clusters of prominent veins that are even tinier than spider veins in an area treated by sclerotherapy. This usually means that reticular veins or other underlying abnormal veins have not been appreciated and treated. Usually, treatment of those veins results in disappearance of the blush.
- Recurrence of spider veins may result from incomplete treatment or because of the underlying predisposition that allows the spider veins to develop in the first place. That is, people with bad veins have bad veins. Treating your spider veins does not prevent more from developing. Hopefully, if you treat new ones every few years you can stay on top of the problem. Also, after child-bearing, which involves great hormonal swings, and after menopause, there may some slowing in the development of new spider veins.