WHAT ARE VARICOSE VEINS?
Varicose veins are veins beneath the skin (spider veins are in the skin) that have become dilated and tortuous (twisting and curling, rather than straight). They are visible as bubbles or snake-like cords under the skin. They may be the size of a telephone cord or as big as your thumb (I’ve seen some larger than lemons!).
They are often uncomfortable, with heaviness, aching, or tiredness developing in the leg with prolonged standing or walking. Some people report itching over the enlarged veins. Sometimes they are sensitive to pressure, as with prolonged sitting. Some people have leg cramps at night, and some have symptoms similar to restless leg syndrome. These symptoms generally reflect the back pressure of blood pooling in the leg veins. I think that is why women have more symptoms than men. Men tolerate the back pressure with fewer symptoms because they generally have more musculature in the legs.
WHAT HAPPENS IF VARICOSE VEINS GO UNTREATED?
Most of our patients with true varicose veins have symptoms of discomfort, and many have some ankle swelling. At the very least, leaving their veins untreated means continued discomfort. We understand varicose veins as a chronic and progressive disease; chronic, meaning ongoing, not going away – people with bad veins don’t stop having bad veins; progressive, meaning there is a tendency for the varicose veins to become more extensive and more uncomfortable over time.
The rate of worsening is not the same for everyone. In general, not treating your varicose veins just means they’ll continue to worsen. As the disease progresses, swelling of the ankle becomes a more prominent symptom. Because of longstanding back pressure down the leg, there is poor capillary flow at the ankle level. That causes deterioration of the health of the skin, with thickening, darkening, and easy skin breakdown and non-healing sores.
These sores are called stasis ulcers. Varicose veins, especially larger ones, can spontaneously clot. This alarms many people because they’ve heard of the dangers of blood clots in the veins. But blood clots in varicose veins rarely extend into the deep veins of the legs where dangerous blood clots occur.
The clotted varicose veins are, however, tender, red, and warm to touch. This is called superficial phlebitis, and is not dangerous, but the tenderness is a nuisance. Sometimes varicose veins cause thinning of the overlying skin to the extent that rubbing against a sheet or with a washcloth results in bursting of the vein. This results in very impressive bleeding, but is easily controlled with light pressure over the vein. While they are not life-threatening emergencies, these latter problems indicate the need for a prompt referral to a vein specialist.
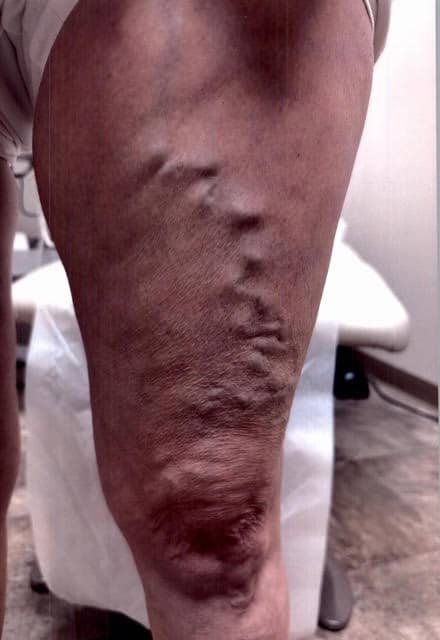
Example of Varicose Veins
Click to enlarge gallery photos & descriptions
WHAT CAUSES VARICOSE VEINS
While there is some controversy in scientific circles about how varicose veins arise, here are some general ideas. First of all, if you have varicose veins, you did not cause them, you were born with a predisposition to develop them. Many people tell me they’ve had jobs that required standing all day long on hard floors. I tell them that it wouldn’t have mattered if they were standing on pillows. Gravity is the enemy, and, unless you’re not ever going to get out of bed, avoiding it is impossible. So, genetics and gravity are the main factors, and you can’t change them. Varicose veins are much more common in women than men, and that’s a factor you can’t change either (at least, not genetically) It is believed that estrogen and progesterone actually promote varicose veins in predisposed women. Pregnancy is often a time when varicose veins make their first appearance. The hormonal changes of pregnancy are probably the main factor. The increased pressure in the pelvis with the enlarging baby contributes, as well. This is also why obesity, which causes higher pressure in the abdomen and pelvis, contributes to varicose vein formation. I have seen a few patients who have developed varicose veins after years of long distance running. I think this is unusual, and not a reason to stop exercise in this way. If you’re a runner, and have varicose veins, just get your veins treated and keep on running.
The common factor in all these settings is pooling in the veins causing abnormal pressure in the surface tributaries. Remember, arteries bring blood from the heart to the legs. So, varicose veins have nothing to do with getting enough blood supply to the legs, or the problems of not getting blood to the legs. Veins return the blood from the legs to the heart. In order to do this, when sitting or standing, the blood must go uphill against gravity – and there is no heart-pump in the feet to assist this. So, there are one-way valves, separated by a few inches, located up the leg veins. These valves open and allow flow up the leg vein in relationship to the heart beat, breathing, and walking. Then they close to prevent pooling down the vein by the force of gravity. The factors mentioned above that are associated with the development of varicose veins all have in common that they result in weakened and failed valves in the veins. Then, the blood does pool down the leg by the force of gravity. That creates a back pressure in the veins that is transmitted out to the surface veins. Because veins are thin-walled and not meant to be exposed to very high pressure, the back pressure causes them to dilate, balloon out, and that becomes a visible varicose vein. As is discussed in the section on varicose vein treatment, you can now understand why it is so important to identify and treat the underlying abnormal veins that are the sources of back pressure into the surface veins that are bothering you.


